When people stop breathing for brief periods while they sleep, it’s called hypopnea. Sleep apnea is diagnosed when a person has multiple episodes of shallow breathing while asleep (hypopneas) and complete cessation of breathing (apneas).
Even if a sleep-related respiratory issue is indicated by a higher-than-average incidence of hypopneas, effective therapies are available. Understanding the origins, manifestations, and consequences of this condition can help in its detection and management.
You are reading: What Is Hypopnea? Common Question And Answers
What Is Hypopnea?
Sleep apnea and other respiratory abnormalities during the night often cause hypopnea as a side effect. When a person’s airflow decreases by at least 30 percent for 10 seconds or longer, we call that a hypopnea. The amount of oxygen in the blood also decreases by at least 3–4% throughout this time. The longer a hypopnea episode continues, the more severe its symptoms.
People with sleep-related breathing difficulties not only have hypopneas, but also apneas, or total stops in breathing, while they are asleep. Sleep apnea is highly probable if a person has five or more hypopnea and apnea occurrences on average per hour of sleep. An untreated sleep-related breathing issue can raise the risk of heart attack, stroke, cardiovascular disease, diabetes, and liver fibrosis, in addition to symptoms including excessive daytime sleepiness and mood abnormalities.
Types of Hypopnea
Three distinct forms of hypopnea have been identified. All hypopneas are episodes of shallow breathing, but the underlying reasons of the various varieties mean that they may need to be treated in different ways. Medical personnel may have trouble determining the specific form of hypopnea a patient is suffering.
- By definition, hypopnea episodes induced by a partial obstruction of the airway are obstructive hypopnea. They are typical of OSA.
- Hypopnea can also occur due to a decreased effort to breathe, a phenomenon known as central hypopnea. It is typical for people with central sleep apnea to experience central hypopnea, which can be brought on by issues in the brain stem or by certain drugs.
- When a person has hypopneas due to a decrease in airflow and a decrease in breathing attempts, they are said to be experiencing mixed hypopneas. A kind of central sleep apnea known as “mixed hypopneas” is common in those being treated for obstructive sleep apnea.
How Is Hypopnea Different From Sleep Apnea?
An apnea is a total cessation of breathing, as opposed to the shallow breathing that occurs during a hypopnea. Breathing events include both hypopneas and apneas. Many different breathing abnormalities manifest themselves during sleep, and the phrase “sleep apnea” is used to describe all of them.
A person is often given a diagnosis of either obstructive or central sleep apnea when they experience more hypopneas and apneas than what is considered healthy. The type of sleep apnea diagnosis given depends on the cause of the apneas and hypopneas.
When a patient has more hypopneas and apneas than normal, a diagnosis of obstructive or central sleep apnea is commonly made. The apneas and hypopneas’ origins inform the diagnosis of sleep apnea.
Symptoms of Hypopnea
If a patient has more hypopneas and apneas than normal, he or she may be diagnosed with obstructive or central sleep apnea. The apneas and hypopneas’ etiology determines the sleep apnea classification assigned.
- Roaring snores
- Excessive drowsiness during the day
- Dissatisfied with the lack of revitalization brought on by waking
- Needing to get up in the middle of the night to use the restroom
- Sleep-related choking and gasping
- Migraine in the morning
- Insufficiency in the sack
- Negative states of mind
- Constant stuffiness in the nose
- Progress in weight growth
Partners of people with sleep apnea may experience sleep disruption from snoring and other symptoms. Anecdotal data reveals that apnea and hypopnea are sometimes only diagnosed when the bed partner of the individual with the disease complains about the snoring and encourages assessment.
Causes of Hypopnea
In obstructive sleep apnea, the airway becomes partially closed, leading to obstructive hypopneas. Obesity and hypothyroidism are two disorders that can contribute to a constricted airway and a more noticeable throat. The size or form of a person’s tonsils or jaw can also contribute to airway narrowing and the development of obstructive hypopneas. Hyperventilation in children is typically caused by enlarged tonsils or adenoids.

Those who suffer from central sleep apnea also have central hypopneas, which occur when the brain momentarily stops sending the body signals to breathe. Central sleep apnea can be brought on by a number of different things, including brain stem damage or the use of opiates or other medications that reduce your ability to relax. Central hypopnea symptoms can also be brought on temporarily by a recent ascent to a high altitude.
Hypopnea Risk Factors
An increased frequency of hypopneas can be brought on by a number of factors:
- Obesity
- Hypothyroidism
- Acromegaly
- This is a disease called myotonic dystrophy.
- The Ehlers-Danlos Syndrome
- Background information
- Under or overbite
- Sexuality in men
- Smoking
Some of them, including obesity or jaw shape, may be direct causes of hypopneas by restricting airflow. However, other factors, like as a person’s sex, may raise their risk.
Hypopnea Diagnosis
As soon as a doctor has reason to suspect sleep-disordered breathing, they will assess risk factors, inquire about the patient’s sleep and health habits, and do whatever diagnostic procedures are necessary. But a doctor is hardly likely to draw the conclusion that there is an increase in hypopneas without first ordering a sleep study. A sleep study, often called polysomnography, is the most reliable method for identifying sleep apnea.
A sleep study provides vital information to sleep specialists, such as the frequency, severity, and duration of apnea and hypopnea events. Additionally, sleep studies aid doctors in distinguishing between obstructive and central sleep apnea.
Although home sleep apnea testing is not common, it is performed in some cases. However, the data collected by home sleep apnea tests is not as comprehensive as that collected by polysomnography. Home sleep apnea testing is recommended by the American Academy of Sleep Medicine only for those at high risk for moderate to severe obstructive sleep apnea and who are otherwise healthy.
Hypopnea Treatment
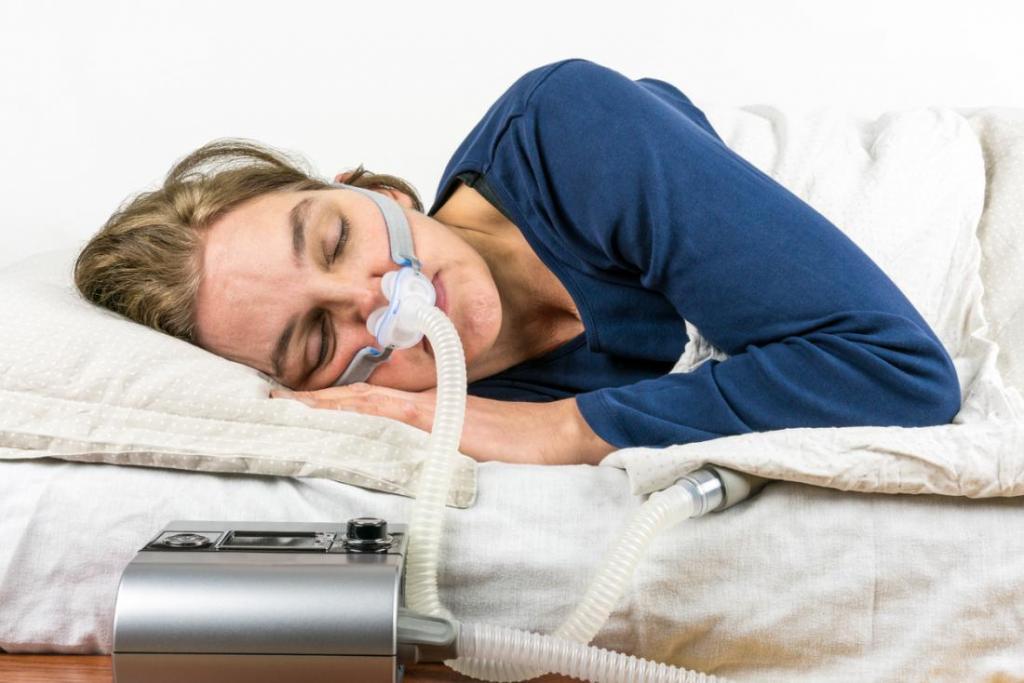
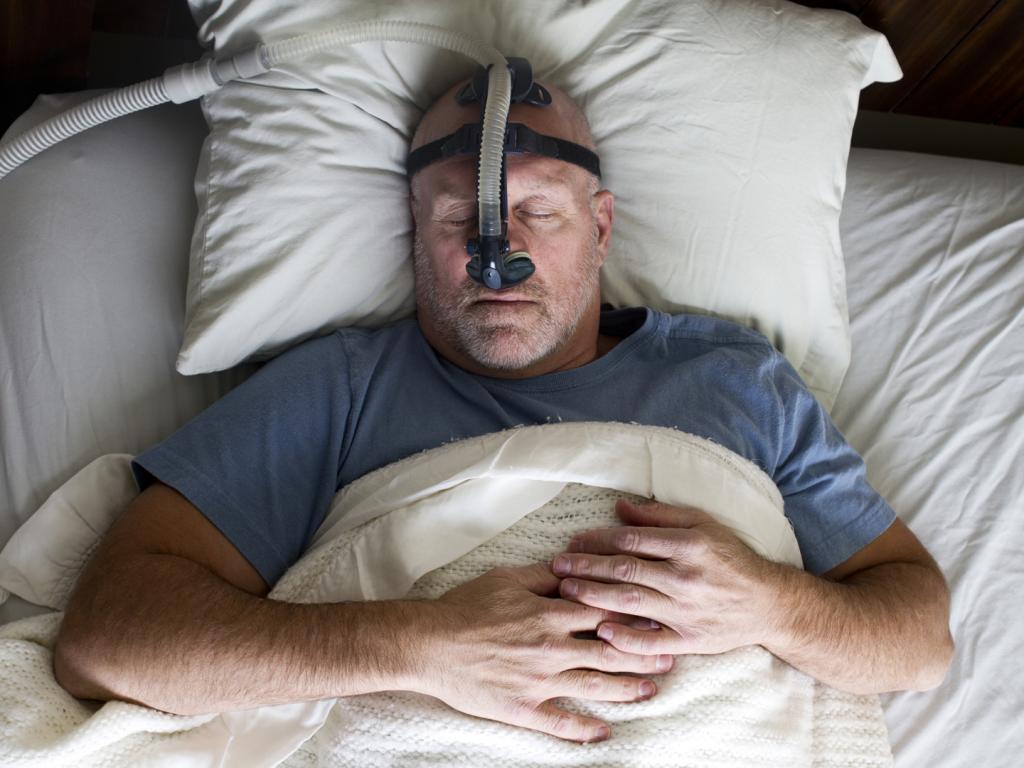
Sleep apnea is characterized by an increase in hypopneas, and is often treated by a combination of lifestyle adjustments and continuous positive airway pressure (CPAP) therapy prescribed by a doctor. Losing weight, cutting back on drinking, shifting your sleeping posture, and quitting smoking are all examples of lifestyle changes that may be beneficial.
While CPAP therapy was originally developed to treat obstructive sleep apnea, it has since been found to be effective in treating central sleep apnea as well. When used in conjunction with a hose and mask, CPAP machines provide continuous positive airway pressure (CPAP) to patients as they sleep in order to maintain an open airway and prevent or significantly reduce the occurrence of hypopnea. Treatment with a CPAP machine that is both effective and used regularly can significantly improve quality of life, as well as lower blood pressure and the likelihood of developing cardiovascular disease.
Occlusive sleep apnea is often treated with CPAP or a similar machine, however an oral appliance or surgery may also be used in some cases. Oral appliances are tools used to move the jaw and tongue forward and improve breathing. Many different operations have been developed to reduce or eliminate airway obstructions.
Hypopnea vs. Sleep Apnea: Similarities and Differences
The amount or quality of breathing during sleep is affected by hypopnea and sleep apnea, two diseases that are quite similar. Both hypopnea and sleep apnea involve breathing difficulties, while sleep apnea causes complete cessation of breathing.
In terms of day-to-day effects, the sole distinction between obstructive sleep apnea and hypopnea is whether the airway is partially or completely blocked. Patients with OSAHS may have both apnea and hypopnea at night, as both diseases are included in the diagnosis. It is for this reason that some academics argue the differences between the two are not substantial enough to require separate study or treatment.
FAQs
What is the main difference between apnea and hypopnea?
Read more : Can You Survive Without Sleep? Common Question And Answers
Both hypopneas and apneas have the same effect on breathing during sleep and are, therefore, extremely similar. Occurring together, sleep apnea and hypopnea are known as obstructive sleep apnea-hypopnea syndrome (OSAHS).
The difference between an apnea episode and a hypopnea episode is that the latter completely stops breathing while the former just disrupts it temporarily. It’s not as serious as apnea because your airway isn’t fully blocked. Complete cessation of breathing for 10 seconds or more is what defines an apnea episode.
Is hypopnea as bad as apnea?
The general consensus is that apneas are more dangerous than hypopneas. An apnea is defined as a disruption of breathing lasting 10 seconds or more. However, hypopneas only cause a mild disruption in breathing.
It stands to reason that the risk and stress on the body are magnified when respiration is completely cut off. Heart disease, obesity, and chronic sleep issues are all possible outcomes of either hypopnea or apnea.
Can hypopnea be cured?
Many cases of hypopnea, especially the milder ones, can be cured by making healthy lifestyle choices and, if necessary, getting medical treatment. A CPAP machine, a healthy diet and regular exercise, or even just a change in sleeping posture can all help.
It may take years of treatment for severe cases of hypopnea to resolve. Surgery, supplemental oxygen, medicine, and the use of a continuous positive airway pressure (CPAP) device are all viable options for treating severe hypopnea.
How many hypopneas per hour is normal?
Hypopneas occur when a person stops breathing completely or almost completely for 10 seconds or longer while sleeping. The average adult has less than five hypopnea episodes each hour. This doesn’t sound like something that requires a doctor’s visit or medication. If you’ve had more than five bouts of hypopnea, it’s time to see a doctor.
What is the apnea-hypopnea score?
The presence and severity of hypopnea or apnea can be assessed by a rating system called the apnea-hypopnea index (AHI). It’s the rate at which you stop breathing while you sleep, in either apnea or hypopnea, expressed as episodes per hour.
Here is how the order pans out:
- Less than five awakenings each hour is considered normal.
- 5-14 hypopneic events per hour is considered mild.
- Approximately 15-30 hypopnea episodes per hour is considered moderate.
- A rate of 30 or more hypopnea episodes per hour is considered severe.
Conclusion
A medical ailment, hypopnea causes periods of interrupted breathing while sleeping. It’s a persistent problem that can be controlled with medication, surgery, or even just a few adjustments to your daily routine. These techniques can help people with hypopnea have better sleep, which in turn improves their overall quality of life.
Rank this thread
Source: https://bestpillowsleepers.com
Category: Sleep Advisors










