A sleep study can help determine the root cause of your sleeplessness if your doctor recommends it. A sleep study, or polysomnography, is a painless examination of your brain’s electrical activity while you’re asleep. It can tell your doctor how much time you spend awake or asleep, how much rapid eye movement (REM) sleep you get, and whether or not you suffer from other symptoms like restless leg syndrome.
What Does a Sleep Study Measure?
The most widely used type of sleep study is a polysomnogram. While you slumber in a high-tech sleep lab that looks like a comfortable hotel room, a technician in a nearby room records your brain activity and selected information from your body. Together, this data reveal a detailed picture of your unique sleep patterns—including how much time you spend in light and deep stages, whether you’re receiving enough oxygen, how often you awaken (even slightly), and whether sleep is disrupted by factors such as arm and leg movements.
You are reading: How Does A Sleep Study Work? A Must Read!
Why Have a Sleep Study?
Polysomnography is the gold standard for sleep studies. In a state-of-the-art sleep lab designed to look like a hotel room, your brain activity and other data are recorded while you sleep while a technician watches over you from another room. The information gathered paints a complete picture of your individual sleep habits, down to the minute details, such as the proportion of time spent in light and deep stages, whether or not you are getting enough oxygen, how often you awaken (even briefly), and whether or not your sleep is disrupted by things like arm and leg movements.
- Sleep apnea is a respiratory problem that prevents you from getting a good night’s sleep by causing you to repeatedly cease breathing throughout the night.
- Narcolepsy causes extreme daytime sleepiness and unexpected bouts of daytime sleepiness.
- Disorder in which you enact your dreams while you’re asleep; also known as REM sleep behavior disorder.
- Like restless legs syndrome, PLM causes you to flex and extend your legs repeatedly during the night.
What Sleep-Lab Equipment Is Used?
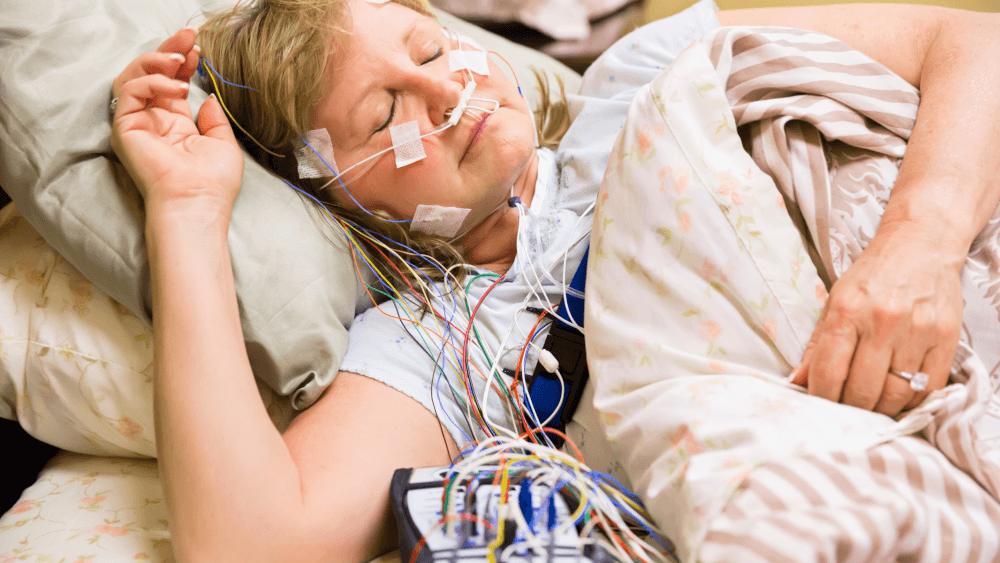
When you first check in at the sleep center (late at night), a technician will use adhesive patches to attach small sensors to your head and body. For freedom of movement while sleeping, the sensors’ connecting wires are typically gathered above your head. Breathing can also be monitored by wrapping an elastic belt over the upper and lower body. Blood oxygen levels can be tracked using a clip attached to a finger or earlobe. In most cases, familiarity develops rapidly.
During the second half of your sleep study in the sleep lab, you may be required to use a continuous positive airway pressure (CPAP) machine if the sleep specialist thinks you have obstructive sleep apnea. To make sure the breathing mask is comfortable and fits properly, you may be requested to wear it for a trial run before turning in for the night. In order to determine whether or not the machine’s adjustments have helped Benjamin’s sleep, the technician will keep an eye on the patient.
What To Expect During a Sleep Study
If you need a polysomnogram, the clinic you visit will provide you with a private room. A technologist will attach painless sensors to your scalp and body before bedtime in order to collect data. The technician will remove the sensors if you need to use the restroom and replace them after you’re done.
In the hours before bed, you can enjoy some quiet time in bed reading or otherwise unwinding. The technologist will keep an eye on your test, write down the results, and be available to answer any questions you may have throughout the night. When you wake up from the sleep study, the monitors will be taken off.
Testing for multiple sleep latency is sometimes administered the day after a polysomnogram. During the duration of five, two-hourly nap times, sensors will record your sleep habits. The technician will alert you that it’s nap time, at which point you can lay down and see if you can nod off.
In home sleep apnea tests, you will receive a device from your doctor and instructions on how to use it. Before bed, follow the instructions for attaching the sensors and turning on the device. Go to sleep at your usual bedtime. The device will collect data throughout the night until you wake up and remove the sensors in the morning.
Sleep Study Results
For sleep apnea testing at home, your doctor will send you home with a machine and detailed instructions. Simply attach the sensors and turn on the device before going to bed. The moment has come for you to get some shut-eye at your regular bedtime. When you turn the gadget on at night, it will continue to gather data until you remove the sensors in the morning.
How To Prepare for a Sleep Study
Read more : How to Make a Mattress Firmer? Easy Step-by-step Guide
Preparing for your sleep study can make the experience more positive and lead to more reliable results.
In advance of your sleep research, you should…
- Discuss all of your prescription choices with your doctor. Don’t skip any medication doses without first talking to your doctor about how doing so might affect the findings of your sleep study.
- Request a tour of the sleep clinic ahead of time if you’re nervous about undergoing a sleep study there. It is possible to have a companion join you throughout the sleep study’s initial setup process.
Before your sleep study begins:
- Proceed as normally as possible.
- Don’t drink any more caffeine after lunchtime.
- Don’t sleep.
- Bring your pajamas, a book, a toothbrush and other necessities, and clothes to change into the next day if your sleep study is being conducted at a clinic. To that end, feel free to bring your own cushion.
What if I Can’t Sleep During a Sleep Study?
As a result of the sensors and the unusual conditions, it is common for people to sleep less during polysomnography than they would otherwise. The findings of your test should not be affected by this, but if you are worried, please discuss it with your doctor.

Types of Sleep Studies
Studies of sleep are conducted to learn more about the processes occurring in the human body while it is at rest. According to the symptoms and potential sleep problems, various sleep investigations can be conducted.
- In a polysomnogram, a patient spends the night in a sleep clinic while being monitored by a trained sleep technologist. Eye movement, brain and muscle activity, respiratory effort and airflow, blood oxygen levels, body placement and movements, snoring, and heart rate are only few of the activities monitored overnight.
- An individual’s ability to fall asleep and reach REM sleep fast during daytime naps is evaluated with the multiple sleep latency test. Excessive daytime sleepiness, whether caused by narcolepsy or anything else, can be diagnosed using this test (idiopathic hypersomnia).
- Adjusting the intensity of continuous positive airway pressure (CPAP) is a typical method of treating sleep apnea. A patient’s required CPAP air pressure is determined during titration by a technician before the device is programmed for at-home use. A second sleep study is typically needed for CPAP titration. A two-night sleep study can be useful when sleep apnea is firmly suspected. Split-night studies employ polysomnography to diagnose sleep apnea and continuous positive airway pressure (CPAP) titration to find the optimal settings for treatment.
- During home sleep apnea testing, a patient’s breathing, heart rate, and other factors are monitored throughout the night. However, home testing does not provide as much information as polysomnography and is not supervised by a technician.
What Can a Sleep Study Diagnose?
Numerous sleep problems can be identified with the help of a sleep study, such as:
- Insomnia
- Apnea in Sleep
- Insomnia of the Legs
- Narcolepsy
- Disorder characterized by recurrent, rhythmic movements of the limbs
- Sleepwalking
- Conversations in the Wee Small Hours (Somniloquy)
- Restless Sleep Behavior Disorder
Who Needs a Sleep Study?
Although sleep studies are often the gold standard for diagnosing sleep disorders, they are not always essential. An individual’s symptoms and general health status are taken into account while deciding whether or not to order a sleep study.
If you’re having trouble sleeping or suffering daytime symptoms like tiredness, depression, or inability to focus, talk to your doctor. Screening for sleep apnea is recommended for obese patients who are experiencing sleep difficulties. If you’re not sure if a sleep study would benefit you, talk to your doctor.
A follow-up sleep study might help your doctor figure out what to do next if you’ve been diagnosed with a sleep disorder but your symptoms haven’t improved despite treatment.
How Much Does a Sleep Study Cost?
Putting a price on a sleep study is tricky. The testing method and the cost associated with the lab determine this. Prices at independent medical facilities tend to be lower than those at large hospital networks. For the most up-to-date details, it’s best to have a conversation with the clinic running your sleep study.
Insurance Coverage for a Sleep Study
Your out-of-pocket expenses will be limited to those not paid for by insurance. Learn if a sleep study is covered by your health insurance by calling your provider.
Read more : What Is A Pack N Play? How Long Can Baby Sleep In Pack N Play?
If your doctor recommends a sleep study but your insurer refuses to pay for it, you may want to investigate your options for appealing the decision. This usually entails proving that the examination is required for medical reasons. Your doctor should be able to assist you in assembling the necessary documentation for your appeal.
Can I Do a Sleep Study at Home?
Current practice limits the use of home sleep tests to diagnose obstructive sleep apnea (OSA). Home sleep apnea tests are less effective at detecting OSA than polysomnography, so the American Academy of Sleep Medicine (AASM) recommends that they only be used when moderate or severe OSA is suspected and when other health conditions are not present. The American Academy of Sleep Medicine also recommends not using an at-home sleep study as the main basis for diagnosing and treating sleep apnea.
Presently, only obstructive sleep apnea may be diagnosed using a home sleep study (OSA). It is recommended by the American Academy of Sleep Medicine (AASM) that home sleep apnea testing only be performed when moderate or severe OSA is suspected and when other health concerns are absent. The American Academy of Sleep Medicine also suggests that sleep apnea shouldn’t be treated based on the results of a home sleep test alone.
The Facts About At-home Sleep Tests
They monitor breathing, not actual sleep.
For the purpose of diagnosing sleep apnea, a sleep study focuses on the patient’s breathing patterns rather than their actual sleep. You can’t expect the sleep test to evaluate things like how long you spend in REM sleep versus non-REM sleep. Instead, it will track how long you go without breathing, how hard you breathe, and how deeply you breathe.
Your doctor needs to prescribe it.
That’s not a simple home test you can get at the drug store. Your family doctor or a doctor at a sleep clinic can prescribe it for at-home use.
It uses sensors to detect breathing patterns.
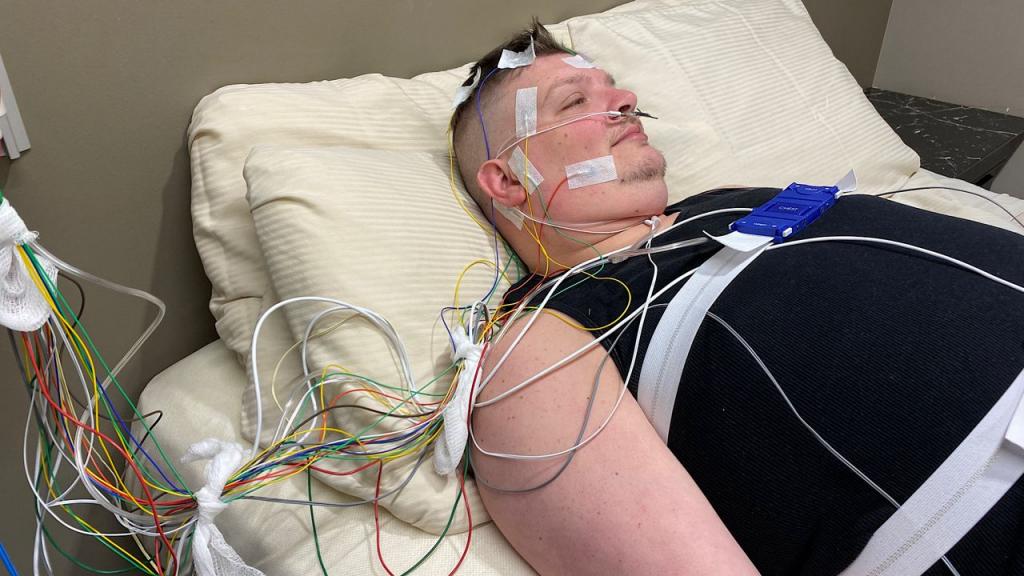
One of the sensors is a finger probe used to determine blood oxygen levels. A second mask, similar to an oxygen mask, will include tubes that you will enter into your nostrils and then wrap around your ears. A number of other sensors are positioned on your chest and belly to record the expansion and contraction caused by your breathing.
It’s a small commitment.
Typically, a single night of use is all that is required for an at-home sleep test. Not only is it more convenient than an in-lab sleep study, but it also costs far less (around a third to a fifth) and is often covered by insurance.
It’s convenient.
A more accurate reflection of your actual sleep patterns may be obtained with an at-home study because you will be in your own familiar environment.
It doesn’t completely rule out apnea.
After the test, your results will be reviewed by a sleep technologist and sent to your physician. If symptoms persist, your physician might recommend an in-lab study. Home tests can sometimes be inaccurate: For instance, your sensors might fall off during the night. At a lab, a physician is on-site to monitor you.
You might have other sleep issues.
Your doctor will receive your sleep study data after they have been reviewed by a sleep technologist. Your doctor may advise a lab test if the symptoms don’t improve. There are a number of factors that can introduce error into a home test, such as the possibility that your sensors will fall off throughout the night. A doctor is available to keep an eye on you while you’re getting your blood drawn.
Have your say on this thread.
Source: https://bestpillowsleepers.com
Category: Sleep Advisors






